Marijuana AnD Mental ILLNESS
|
Numerous studies have demonstrated a strong correlation between marijuana use and Metal Illness. Over these past several years the association has now been proven beyond just a correlation. Depending upon several characteristics and elements – science has now proven that marijuana use is a causative factor for Mental Illness.
First, look at the work of the American Psychiatric Association (APA). After a 12 year field study, the American Psychiatric Association (APA) found that: a) Eight psychiatric mental disorders were caused by cannabis use, including: Anxiety Disorders; Depression; Bipolar Disorder; Schizophrenia; Amotivational Syndrome; Disruptive Cognitive Functioning; Neuropsychological Decline; and, Psychotic Disorders. b) And in terms of comorbidity the APA found that between 50% and 90% of cannabis-dependent persons are diagnosed with an affective disorder, suicidality, or an anxiety disorder; and cannabis use is associated with poorer life satisfaction, increased mental health treatment and hospitalization, and higher rates of depression, anxiety disorders, suicide attempts and conduct disorder. c) The APA also found that cannabis use is highly related to other secondary substance use disorders (74%); and is often quite commonly found with major depressive disorders (11%), and anti-social (30%), obsessive-compulsive (19%), and paranoid (18%) personality disorders. Again, by definition, the APA found that cannabis is a dangerous drug and is a causative factor for mental illness and this research has been confirmed by numerous studies including those through the National Institute of Drug Abuse, all of which clearly demonstrate not just correlation but causation between marijuana use and mental disorders. Reference: Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, DSM-V, American Psychiatric Association. Reference: Journal of Addiction Research & Therapy, Marijuana Addictive Disorders: DSM-5 Substance-Related Disorders, Norman S Miller, Thersilla Oberbarnscheidt, and Mark S Gold. |
|
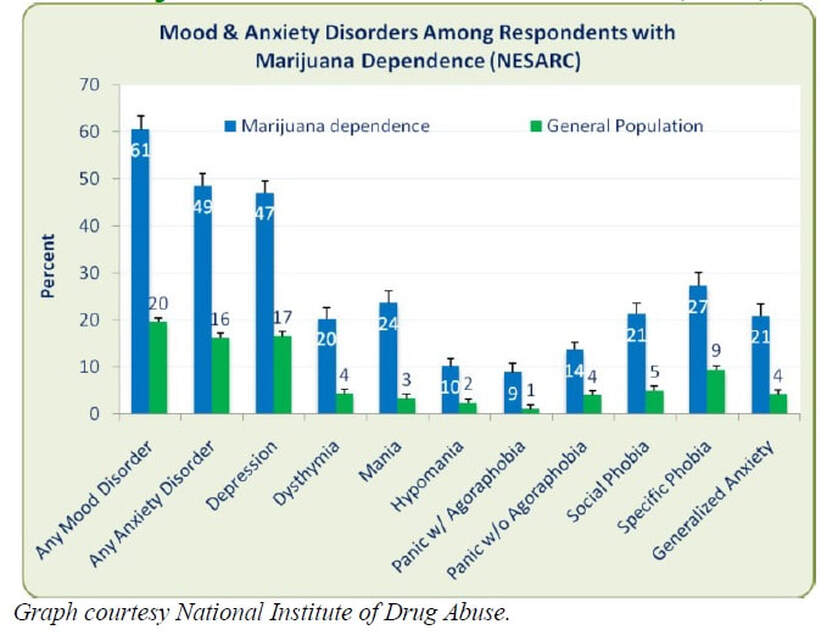
Research has long implicated cannabis as an exacerbating factor in mental illness where mental illness and/or personality problems are pre-existing or concurrent conditions. Recent research has largely supported these earlier findings but also implicates a role of marijuana with anxiety disorders, mood disorders and depression.
One study found that the severity of depression, anxiety and alexithymic symptoms increased progressively with the degree of involvement with cannabis, and chronic use of cannabis was associated with a high prevalence of co-morbid psychiatric disorders. Other studies demonstrated that:
Other studies have implicated marijuana use in depression; panic reactions and suicide; and anti-social personality characteristics. Cannabis-related mental disorders are quite serious, and many people find themselves as chronic clients in mental health programs or as Mentally Ill Chemical Abusers (MICAs) because of the effects of marijuana. Early use of marijuana has been shown to double the risk of someone developing schizophrenia and other psychoses - including mania and bipolar disorder - and mood disorders. Also, it can worsen psychotic symptoms for those already ill, and trigger relapse. Several studies back this up. Less dramatic, but also troubling, are effects of cannabis on acute or chronic impairment of attention, memory and psychomotor performance. These effects can contribute to reduced functioning and a lower quality of life, as well as an increase in accidents and injuries. |
|
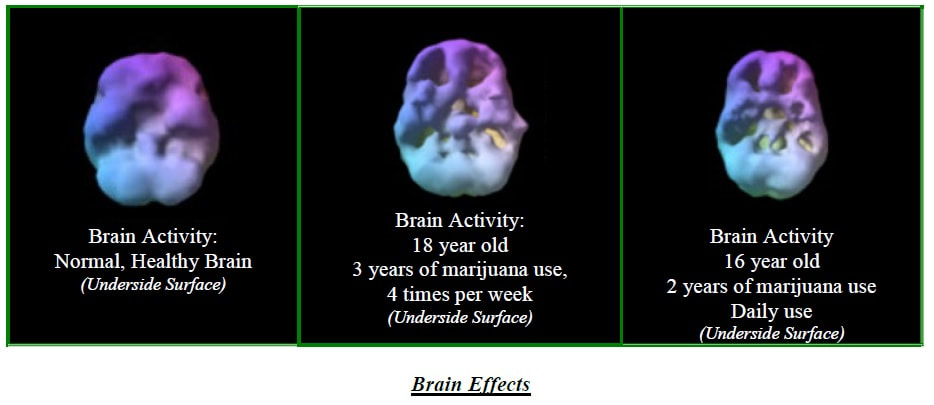
The effects of smoking marijuana typically cause decreased activity in the posterior temporal lobes bilaterally. The damage can be mild or severe, depending on how long a person used, how much use occurred, what other substances were used and how vulnerable a particular brain is.
Reference: “High Resolution Brain SPECT Imaging - Marijuana Smokers with AD/HD”, Daniel Amen, M.D., Journal of Psychoactive Drugs, Volume 30, No. 2, April-June 1998. |
It affects the brain. It has immediate effects - some of which are negative and it has long term effects – both adverse effects and other side effects – both subtle and some more pronounced, depending upon bio-psycho- social variables. |
|
RESOURCES:
Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, DSM-V, American Psychiatric Association. Journal of Addiction Research & Therapy, Marijuana Addictive Disorders: DSM-5 Substance-Related Disorders, Norman S Miller, Thersilla Oberbarnscheidt, and Mark S Gold. “Marijuana – Medical Implications” (John R. Hubbard, M.D., Ph.D., Sharonee E. Franco, M.D., and Emmanuel S. Onaivi, Ph.D., Vanderbilt University School of Medicine, Nashville, Tennessee, American Family Physician, December 1999); Psychiatric Symptoms in Male Cannabis Users not using other Illicit Drugs, Troisi, Pasini, Saacco, Spalletta, Addiction, 93(4) April 1998; Cannabis use correlates with schizotypy in healthy people, Williams, Wellman, Rawlins, Addiction, 91(6), June 1996; The human toxicity of marijuana, Nahas, Latour, Medical Journal of Australia 156(7), April 1992; Marijuana use, introspectiveness, and mental health; Zablocki, Aidala, Hansell, White; Journal of Health and Social Behavior 32(1); March 1991; Substance-dependent, conduct-disordered adolescent males: severity of diagnosis predicts 2-year outcome, Crowley, Miikulich, MacDonald, Young, Zerbe, Journal of Drug and Alcohol Dependence, 49(3), February 1, 1998; Treated delinquent boys substance use: onset, pattern, relationship to conduct and mood disorders, Young, Mikulich, Goodwin, Hardy, Martin, Zoccolillo, Crowley, Journal of Drug and Alcohol Dependence, 37(2) February 1995; Correlates of Depression in Primary Care, Rowe, Fleming, Barry, Manwell, Kropp, Journal of Family Practice, 41(6), December 8, 1995; Health aspects of cannabis, Hollister; Journal of Pharmacological Review, 1986, 38(1); The general pharmacology of cannabinoids in eds Cannabis and its derivatives, Paton, Pertwee, Temple, Oxford University Press, 1972; Neurobiology of marijuana abuse, Abood, Martin, Trends in Pharmacological Sciences, 13(5), May 1992 (9); The association of anti-social personality symptoms with marijuana abuse/dependence. A Monozygotic co-twin study, Scherrer, Lin,Eisen, Goldberg, True, Lyons, Tsuang; Journal of Nervous and Mental Disorders; 184(10); October 1996; Anti-social behavior: Its relation to Selected Sociodemographic Variables and Alcohol and Drug Use Among Mexican Students, Substance Use and Misuse, Vol 33 (7) 1998; Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, American Psychiatric Association, 1994; Sewell, R.A., Ranganathan, M., & D'Souza, D.C.(2009). Cannabinoids and psychosis, International Review of Psychiatry, 21(2), 152-162; Barkus, E., & Murray, R. M. (2010). Substance use in adolescence and psychosis: clarifying the relationship. Annual Review of Clinical Psychology, 6, 365-389 doi:10.1146/annurev.clinpsy.121208.131220; Matthijs, N., Touquet, G., & De Hert, M. (2009). [Cannabis-induced mania? A case study and literature review]. Tijdschrift Voor Psychiatrie; Degenhardt, L., Hall, W., & Lynskey, M. (2003). Testing hypotheses about the relationship between cannabis use and psychosis. Drug and Alcohol Dependence; Moore, T.M., Stuart, G.L., Meehan, J.C., Rhatigan, D.L., Hellmuth, J.C., & Keen, S.M. (2008). Drug abuse and aggression between intimate partners: A meta-analytic review. Clinical Psychology Review; Hall, W. & Solowij, N. (1998). Adverse effects of cannabis. Lancet, 352(9140), 1611-1616. |